Doctor on Call : Psoriasis
|
Dr Ronald Vender, Associate Clinical Professor, Division of Dermatology, Department of Medicine, McMaster University, Hamilton, Ontario and Founder and Director of Dermatrials Research Inc. bh IN BRIEF In addition to teaching at McMaster University, Dr. Ron Vender is a dermatologist who currently practices in Hamilton, Ontario, and is the founder and director of Dermatrials Research Inc. He has participated as principal investigator in over 80 clinical trials. He was also Head of the Division of Dermatology, Department of Medicine, at St. Joseph’s Healthcare in Hamilton, as well as an active staff and dermatology consultant. He is one of eight Canadians elected to the International Psoriasis Council, and a member of the Canadian Professors of Dermatology and the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis. He has published widely and serves on the editorial board of the Journal of Cutaneous Medicine and Surgery as well as the Journal of Clinical & Experimental Dermatology
|
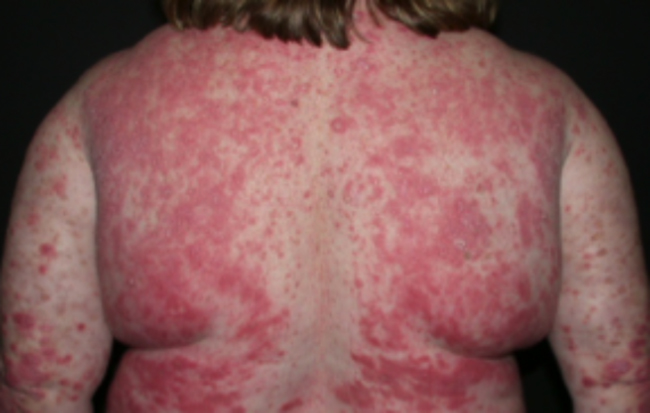
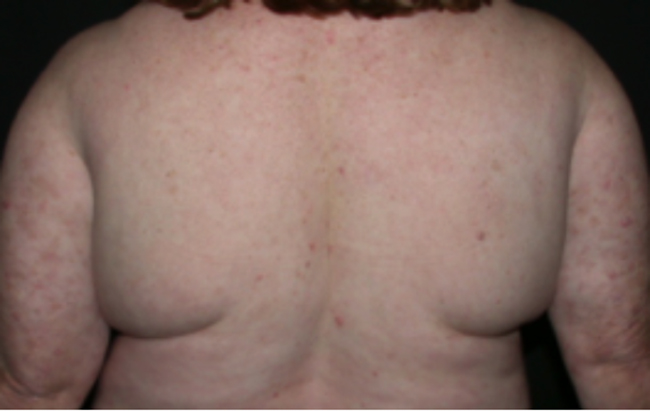
1. What is psoriasis?Psoriasis is a non-contagious, autoimmune disease that affects patients in physical and psychosocial terms. It affects families because of the patient’s need for psychosocial support and, in the workplace, it results in reduced productivity. 2. Is Psoriasis linked to other diseases?Psoriasis is a systemic disease that is visible as a skin condition but it is also associated with psoriatic arthritis, inflammatory bowel disease, diabetes, hypertension, anxiety and depression. If it is treated early and effectively there is likely to be a decrease in such associated diseases because treating it early and effectively can reduce the impact of other diseases or complications. 3. Can psoriasis be cured? Do treatments impact the workplace?Psoriasis has no cure but it can be controlled. Basically, there are four treatment options: topical, traditional systemic medications taken orally, phototherapy, and newer biologics delivered by infusion or needles. Biologics are basically synthesized antibodies to the enzymes that are believed to make psoriasis worse. They allow the patient to function normally and are not time-consuming to administer. Treatment options impact the workplace. In fact, when a patient is not being treated with the most effective treatment option, more than one workplace may be affected. For example, consider a patient who needs to apply topical medicine to the scalp twice a day, a process that takes about two hours and interferes with workplace activities. Then, consider that the patient may need help, for example, when arthritis makes it impossible for the patient to apply the required creams and lotions, or when the patient must be driven to a physician’s office for ultraviolet phototherapy. In these cases, it is likely that neither the patient nor the partner or family member can hold a full-time job. In contrast, think of the patient being treated with a biologic that is self-administered in a matter of minutes, wherever the patient is, without help from anyone, and with no impact on any workplace or productivity. 4. Are there issues in accessing treatment?There are two main issues associated with accessing treatment. The first, relates to finding a dermatologist who is interested in psoriasis and has experience treating it. The second is cost. Although biologics can seem quite expensive, they are actually very cost effective. The patient can work during treatment. Comorbidities are reduced because biologics reduce systemic inflammation. The patient gets better more quickly and stays better longer. Treatment is safer, workplace productivity is not affected, and overall health care costs are lower. 5. At what point in a patient’s disease would you initiate a biologic?Generally, a biologic is indicated for patients with moderate to severe disease which usually means that a minimum of 10% of the body is covered with psoriasis or the disease is affecting difficult to treat places such as the face, soles or palms, or other sensitive areas on the body. A biologic is also indicated if psoriasis is associated with another condition, such as arthritis or inflammatory bowel disease. A biologic would also be considered if the disease is affecting a patient’s productivity at work or overall quality of life. Research has shown that biologics improve quality of life. By quality of life, I mean the ability to interact socially, participate in sports, interact intimately with partners, go swimming, wear shorts and generally, participate without embarrassment in activities of daily life that normal people take for granted. People who do not suffer from psoriasis should realize that it is not contagious and affects people on the inside and outside. Friends and coworkers should show compassion and recognize that people with psoriasis need their help and support. |